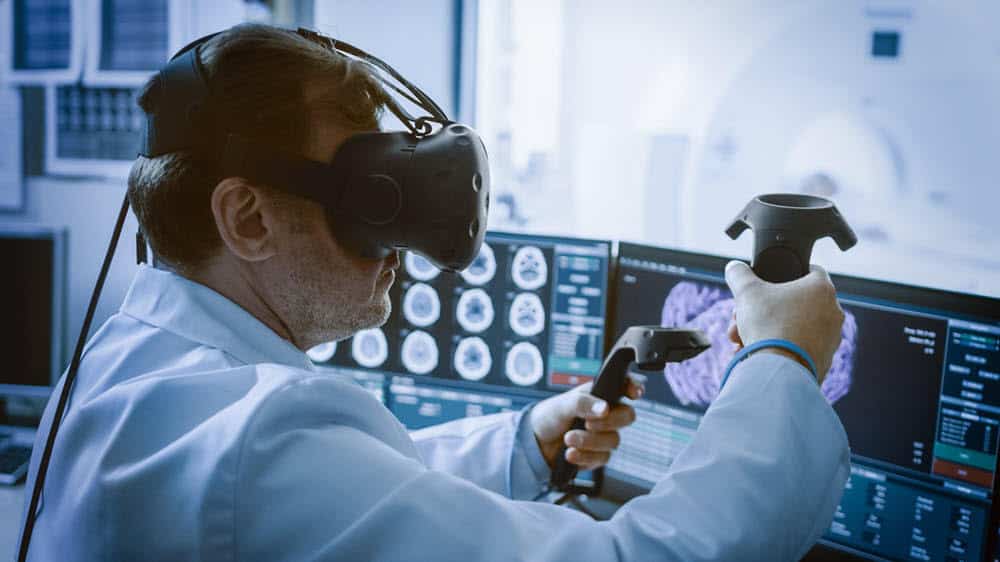
Virtual reality (VR) is an emerging technology that is showing great promise for enhancing mental health treatments. VR involves the use of computer-generated simulations to create immersive, three-dimensional environments that users can interact with in realistic ways (Rizzo et al., 2017). In recent years, VR has become more affordable, accessible, and sophisticated in its capabilities, leading to growing interest in its clinical applications for mental health disorders (Freeman et al., 2017). This technology may provide new avenues for assessment, treatment delivery, and training of clinicians that could significantly advance the field.
VR for Assessment and Diagnosis
VR environments can be designed to simulate real-world situations in order to observe patient behaviors and make clinical assessments in ecologically valid settings (Parsons & Carlew, 2016). For example, VR social situations have been created to assess social cognition and skills in populations with social anxiety, autism spectrum disorders, and schizophrenia (Smith et al., 2015). VR allows clinicians to systematically control and manipulate social stimuli and analyze resulting behaviors and physiological reactions. This can provide valuable information about symptoms and functioning that may be difficult to obtain through traditional assessment methods.
VR for Treatment Delivery
A growing body of research has demonstrated the effectiveness of VR for delivering exposure therapy, particularly for treating anxiety disorders. VR allows patients to confront fears in a graduated, controlled way within simulations of real-world environments (Opris et al., 2012). Systematic reviews have found VR exposure therapy to be as effective as in-vivo exposure across a range of anxiety disorders, including phobias, PTSD, and panic disorder (Carl et al., 2019). VR treatments have also shown preliminary effectiveness for other conditions such as eating disorders, addiction, chronic pain, and depression (Rizzo & Shilling, 2017). A key advantage of VR is that it allows treatment to occur within the clinician’s office rather than requiring real-world trips that may be difficult to arrange.
VR for Training Mental Health Professionals
VR simulations hold promise for training clinicians and healthcare professionals in skills that are challenging to teach through traditional methods (Kramer et al., 2015). Trainees can practice clinical techniques and decision-making within virtual environments that emulate realistic clinical scenarios with simulated patients. This allows them to gain experience and receive feedback in a safe, controlled setting. Early research suggests VR training can improve psychiatric skills such as administering cognitive assessments, recognizing symptoms, practicing CBT techniques, and responding to suicidal patients (Wise et al., 2019). VR training environments may provide an efficient supplement to standard clinical supervision and mentoring models.
Current Limitations and Ethical Considerations
Despite its promise, there are a number of limitations to the adoption of VR for mental healthcare. The costs of equipment and software development remain high for many clinics and researchers (Botella et al., 2015). Evidence for clinical effectiveness remains preliminary in some areas, underscoring the need for more rigorous, controlled studies. It will also be critical to establish protocols that ensure ethical use of VR, such as managing risks of simulation sickness and carefully considering applications that involve deception or potentially harmful content (Madary & Metzinger, 2016). Finally, many practical issues must still be addressed related to workflows, training requirements, and determining appropriate applications of this technology among populations most likely to benefit.
Here are some key current limitations and ethical considerations around the use of virtual reality for mental health assessment and treatment:
Limitations
- Cost and access – VR headsets and software are still relatively expensive and not widely accessible. This limits the ability for VR to be implemented on a large scale in clinical settings right now.
- Developing evidence base – More research is needed to establish the reliability, validity and efficacy of VR assessments and treatments. The evidence base is still emerging.
- Technical challenges – There are ongoing technical issues around things like achieving truly immersive VR experiences, cybersickness, and making experiences realistic. These can impact the effectiveness of VR.
- Attrition – Dropout rates from VR treatments can be high. Ensuring ongoing engagement is a challenge.
Ethical Considerations
- Privacy and confidentiality – Collecting data on individuals’ behaviors, physiology etc. during VR raises privacy issues. Proper data governance needs to be ensured.
- Reality distortion – VR can blur the lines between real and virtual worlds, which may have unintended psychological consequences, especially for those with mental health conditions affecting reality testing.
- Long-term effects – The long-term physical and psychological effects of prolonged VR exposure are unknown. This raises precautionary concerns.
- Informed consent – Given potential risks, fully informed consent is critical when using VR for mental health assessment and treatment.
- Access and equity – There are concerns about costs limiting access to VR for mental health purposes, exacerbating disparities.
- Ethical oversight – Clear protocols and oversight are needed as the use of VR for mental health expands, to ensure it is done responsibly.
Conclusion
Immersive VR environments have the potential to transform assessment, treatment delivery, and clinical training practices in mental healthcare. The capacity to simulate realistic situations with a high degree of control enables interventions and experiments that are not possible with traditional methods. Despite current limitations, rapid technological progress combined with a growing evidence base suggests VR will likely have an expanding role in mental health treatments moving forward. Careful research and ethical deliberation will be key to ensuring this emerging technology is leveraged to effectively enhance clinical care and outcomes for patients.
References
Botella, C., Fernández-Álvarez, J., Guillén, V., García-Palacios, A., & Baños, R. (2017). Recent progress in virtual reality exposure therapy for phobias: A systematic review. Current psychiatry reports, 19(7), 42.
Carl, E., Stein, A. T., Levihn-Coon, A., Pogue, J. R., Rothbaum, B., Emmelkamp, P., … & Powers, M. B. (2019). Virtual reality exposure therapy for anxiety and related disorders: A meta-analysis of randomized controlled trials. Journal of anxiety disorders, 61, 27-36.
Freeman, D., Reeve, S., Robinson, A., Ehlers, A., Clark, D., Spanlang, B., & Slater, M. (2017). Virtual reality in the assessment, understanding, and treatment of mental health disorders. Psychological medicine, 47(14), 2393-2400.
Kramer, M. K., Williams, S. C., & Ferrin, D. L. (2015). Using virtual simulated patients to train health care professionals to recognize mitigating factors in patient aggression. Journal of medical Internet research, 17(11), e262.
Madary, M., & Metzinger, T. K. (2016). Real virtuality: a code of ethical conduct. Recommendations for good scientific practice and the consumers of VR-technology. Frontiers in robotics and AI, 3, 3.
Opris, D., Pintea, S., Garcia-Palacios, A., Botella, C., Szamoskozi, S., & David, D. (2012). Virtual reality exposure therapy in anxiety disorders: a quantitative meta-analysis. Depression and anxiety, 29(2), 85-93.
Parsons, T. D., & Carlew, A. R. (2016). Bimodal virtual reality stroop for assessing distractor inhibition in autism spectrum disorders. Journal of autism and developmental disorders, 46(4), 1255-1267.