hePatients today have more access to healthcare than ever before, thanks in large part to technology, The quality of care is improving along with patient outcomes. In addition, more people can receive care promptly. As a result, healthcare overall has become smarter, more effective, and more personalized. How is this being accomplished?
Electronic Health Records
Electronic health records (EHRs) are having a major impact on healthcare in several key ways. They improve access to patient data for better care quality and patient safety. Although EHR adoption requires major upfront investments, studies show they can lead to cost efficiencies through reduced paperwork, improved coordination, lower rates of duplicative testing, and more. However, realizing savings depends on proper system use and information exchange.
Features like patient portals allow patients to directly access their test results, contact providers, refill medications, schedule appointments, and more. This facilitates patient self-management and shared decision-making. Aggregated EHR data aids understanding of treatment effectiveness, patient outcomes, and population health trends. This “big data” can inform improvements at systemic levels beyond the point of care. However, privacy and ethical use concerns exist.
Properly developed, implemented, and effectively used, EHRs promise to support improved population health and transform healthcare delivery. Adoption has increased substantially but barriers like usability issues, interoperability challenges, and changing clinical workflows remain as healthcare aims realize EHRs’ full potential.
heaalth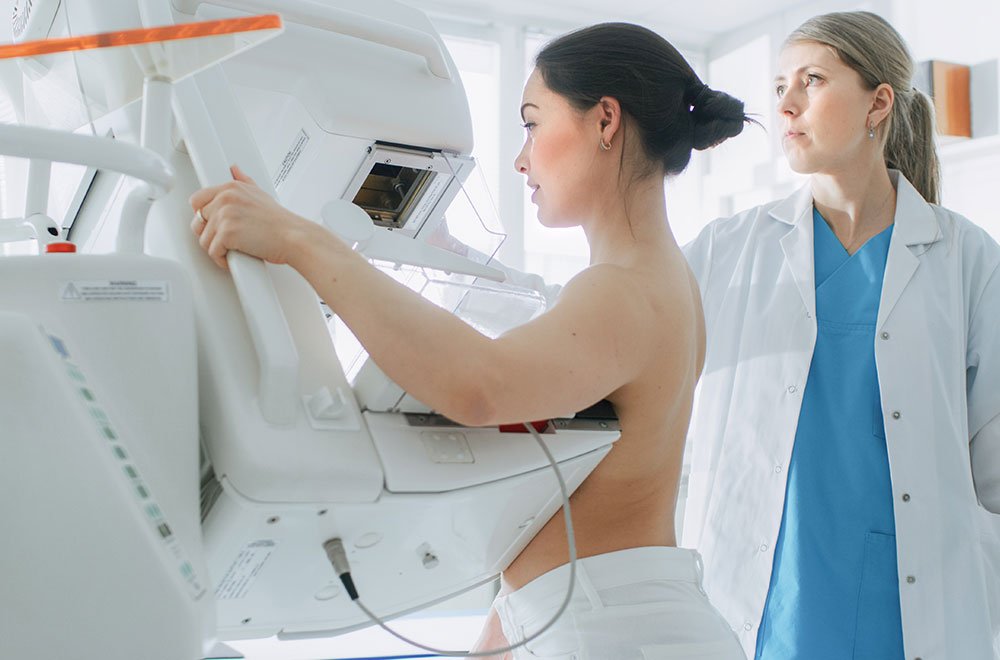
Telemedicine
Telemedicine became popular during the global pandemic. People found they could use telecommunications technology to better their health without ever leaving home, and this trend continues today. Video conferences, phone calls, and text messages allow them to get the care they need promptly, even when other factors prevent them from seeing a doctor in person. While telehealth providers must go through the telehealth licensing process, most organizations find doing so is beneficial.
Rural and underserved communities remain the biggest beneficiaries of this technology. Patients no longer need to travel for hours to get quality healthcare. They can see experts from across the globe while sitting in their homes. This technology helps reduce healthcare disparities. It also brings travel costs related to healthcare under control.
Telemedicine removes many barriers to medical access. It can overcome both technology and mobility constraints. At the same time, it helps to bring healthcare costs down. As more medical professionals across the globe adopt this technology, things will only improve. More people will have access to excellent care, regardless of their social status, location, and more. This will lead to better healthcare outcomes for all.
Remote Monitoring
Medical professionals can track patient health data from afar with the help of wearable devices. These devices provide real-time updates on vital signs. If changes are detected, the doctor receives an alert. They can then intervene.
These remote monitoring tools allow chronically ill patients to better manage their health from the comfort of their homes while avoiding unnecessary trips to hospitals or doctor’s offices. For example, a cardiac patient’s internet-linked pacemaker automatically transmits cardiac rhythms to their physician, who reviews the data for disturbances. If irregular heartbeats start occurring, medication adjustments can be made right away instead of after the patient reports issues at the next appointment.
Other home-based devices like internet-connected glucometers for diabetes patients relay blood sugar numbers to care teams. This helps calibrate treatment plans to minimize hyper/hypoglycemic episodes. Providers also set parameters so they’re notified if readouts fall outside specified zones, enabling rapid medical response.
The convenience and independence of remote healthcare monitoring improve patient outlooks about their disease management ability. The constant data flow allows physicians to deliver truly personalized, timely, and efficient care. The patient/provider relationship will change even more as this technology makes its way into more aspects of healthcare in the coming years.
Artificial Intelligence
Artificial intelligence (AI) also holds great promise for revolutionizing medicine. AI systems can scan and interpret medical images, identifying potential issues faster and more accurately than the human eye. An AI algorithm was recently found to detect breast cancer from mammograms 30 times faster than doctors while reducing the cancer miss rate by 9%. AI can also help diagnose complex conditions and create tailored treatment plans by assessing a patient’s medical history, genetics, and symptoms. Clinical decision support systems that apply AI can provide instant guidance on medications, tests needed, and patient risk factors.
Robotics
Robotics too is advancing rapidly in the healthcare realm. Robots can assist in surgeries allowing greater precision and flexibility than conventional techniques. Smaller incisions from robotic procedures typically lead to shorter hospital stays for patients. Some robots also use AI to continuously adapt techniques based on surgical outcomes and new research.
Robots are being used in hospital pharmacies today. When they are, medical errors decrease. In addition, automation in medication packaging and disbursement improves. Many hospitals also use disinfection robots along with conventional cleaning methods. These robots use UV light to help minimize hospital-acquired infections.
Data Analytics
Moreover, technology gives both patients and providers faster access to important health data that can inform better decision-making. Predictive analytics tools powered by AI can determine patients’ risk likelihood for conditions like heart disease, stroke, or diabetes. This enables earlier lifestyle and treatment interventions. Big data analytics also help researchers detect new disease correlations by assessing huge sets of population health data. By gathering real evidence about the effectiveness of various clinical approaches, data science facilitates greater quality and consistency of care.
Challenges and Accessibility
Of course, new technology also raises important challenges around ethics, privacy, accessibility, biases, and appropriate integration into clinical workflows. Extensive testing and validation are required to ensure AI systems make recommendations that align with guidelines accepted by healthcare experts. Appropriate protocols must likewise govern the sharing and security of confidential patient information in digital platforms. Not all populations benefit equally from technological innovations due to limited tech familiarity, internet availability, or disadvantages faced by marginalized groups. Concerted efforts are therefore needed to increase digital literacy and access.
Though introducing new workflows and requiring updated skills, technology undeniably has vast potential to improve healthcare services, outcomes, and the patient experience. From tiny medical sensors and robots to cognitive computing, the healthcare transformation driven by advanced innovations has only just begun. If solutions evolve carefully according to doctor and patient needs, technology can help create a healthcare future with greater connection, customization, and active management of personal health.